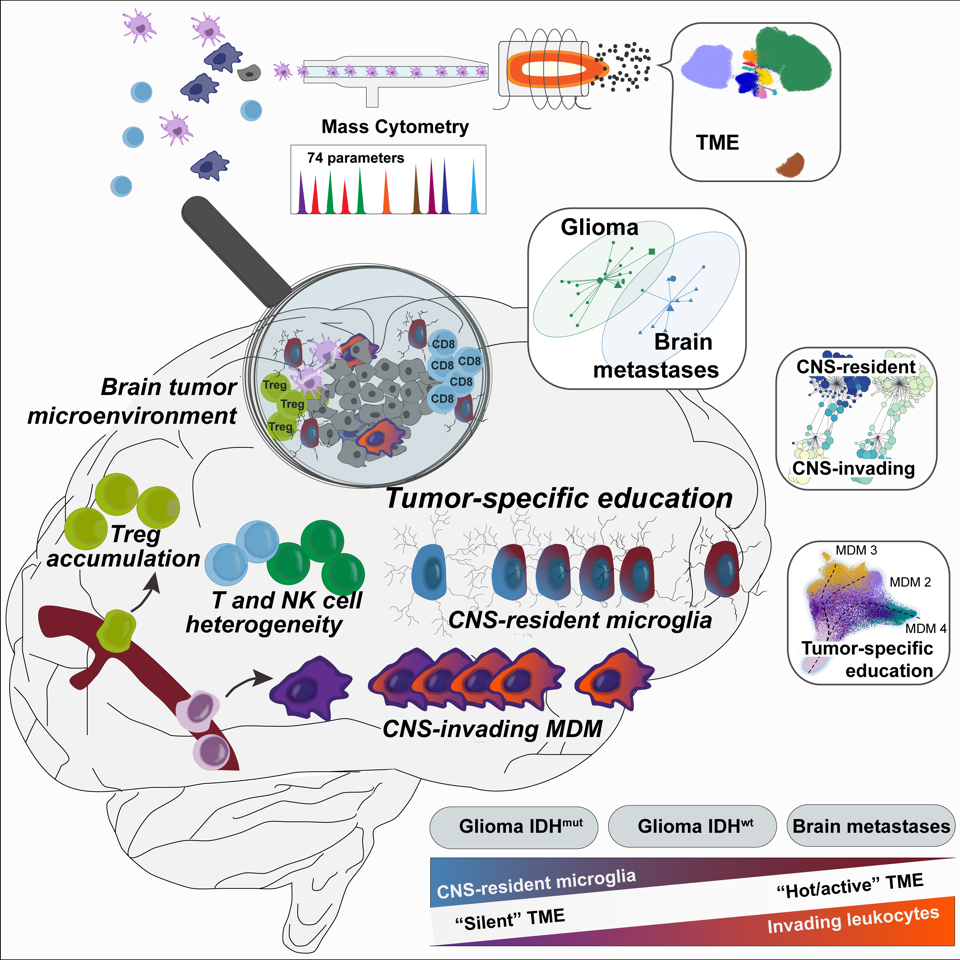
Mapping Immune Cells in Brain Tumors
The removal of a malignant brain tumor is something of a balancing act between removing as much tumor tissue as possible at the same time as protecting the healthy tissue. Since cancer cells infiltrate healthy brain tissue, it is often not possible to remove brain tumors completely during surgery. After an operation that removes as much of the tumor as possible, the prognosis can be improved by subsequent radiotherapy and chemotherapy, but a cure with conventional treatments is difficult to achieve.
Hope through immunotherapy
A team of researchers at the University of Zurich (UZH) and the University Hospital Zurich (USZ) has now found what types of immune cells are present in what numbers in different types of brain tumors. These very precise “tumor maps” are essential to gain a better understanding of the individual immune components in the tumor and to develop targeted immunotherapies that activate an immune defense reaction.
“Our immune system is very precise and efficient. The immune defense can eliminate individual tumor cells, while protecting healthy cells,” explains Burkhard Becher of the Institute of Experimental Immunology at the University of Zurich. Immunotherapy can have astonishing success in treating some types of cancers – but with malignant brain tumors, immunotherapy has thus far yielded disappointing results. One of the reasons for this is previously, that the composition of the tumor tissue in brain tumors, specifically regarding to immune cells, was not explored with sufficient detail.
High-dimensional mass cytometry and complex computer algorithms
To characterize the immune cells in malignant brain tumors, the researchers analyzed tissue from the neurosurgery operating theaters of USZ using a method established at UZH called high-dimensional mass cytometry. This technology makes it possible to analyze millions of different cell types at the same time at the single cell level. The cells are characterized using numerous proteins on their surface and in the cell interior, which vary according to the cell type. The huge amount of data is then processed with complex, self-learning computer algorithms. “For every brain tumor, our technology gives an individual signature of the immune cells present. Similarities and differences between patients and tumor types can thus be compared,” says Burkhard Becher.
Immune cell composition depends of the type of tumor
The study shows that it is primarily the tumor type which determines the kind, frequency and distribution of immune cells present in individual brain tumors. “Gliomas, which develop directly in the brain, look different from metastases of other tumors in the body which have spread into the brain. In gliomas too we can clearly differentiate between various sub-groups through the specific composition of the immune cells,” add Ekaterina Friebel and Konstantina Kapolou, both PhD candidates in the collaborating research groups.
According to Marian Christoph Neidert, neurosurgeon at USZ, the results are not only helpful for better understanding the immunological mechanisms in brain tumors: “They also offer a basis for the development of immunotherapies that are tailored to the various types of brain tumors.” The tumor tissue investigated in the study came from patients treated at the USZ Brain Tumor Center. However, further research work is still required before brain tumor patients will be able to benefit from the immunological findings.
Literature:
Ekaterina Friebel, Konstantina Kapolou et all: Single-cell mapping of human brain cancer reveals tumor-specific instruction of tissue invading leukocytes. Cell, 28 May 2020. DOI: 10.1016/j.cell.2020.04.055